- Joined
- Nov 17, 2015
- Messages
- 13,949
except....
"Their findings are preliminary, still being compiled and have not been published in a peer-reviewed journal -- but some not involved with the study called the results a breakthrough."
except....
"Their findings are preliminary, still being compiled and have not been published in a peer-reviewed journal -- but some not involved with the study called the results a breakthrough."
Researchers in England said they have the first evidence that a drug can improve COVID-19 survival: A cheap, widely available steroid called dexamethasone reduced deaths by up to one third in severely ill hospitalized patients.
The results were announced Tuesday and the British government immediately authorized the drug's use across the United Kingdom for coronavirus patients like those who did well in the study. Researchers said they would publish results soon, and several independent experts said it's important to see details to know how much of a difference the drug, dexamethasone, might make and for whom.
But “bottom line is, good news,” said the United States’ top infectious disease expert, Dr. Anthony Fauci. “This is a significant improvement in the available therapeutic options that we have.”
The study, led by the University of Oxford, was a large, strict test that randomly assigned 2,104 patients to get the drug and compared them with 4,321 patients getting only usual care.
Reisman knew about a post-COVID trial for survivors of mild to moderate COVID-19 symptoms. Riley enrolled in the clinical trial for leronlimab, a drug that was originally developed to treat HIV, but is showing promise in the coronavirus fight. He had four injections in his stomach over two weeks.Riley said he immediately felt better. He returned to a faster pace, his blood pressure returned to normal and the other symptoms – the anxiety, the insomnia — faded.
Dr. Chris Recknor, a Gainesville internist who runs one of the six sites for the leronlimab clinical trial, is also a COVID-19 survivor.(snip)
His physician at the hospital obtained “compassionate use” permission from the Food and Drug Administration to prescribe leronlimab. Recknor said he felt better within two days after getting the medication and has fully recovered.“The only way I can explain it is, it was like it felt like I had 1,000 cups of coffee,” said Recknor. “And then after the medicine, it was like a relaxing time on the beach. A couple days after the medicine, I was back to doing everything normal.
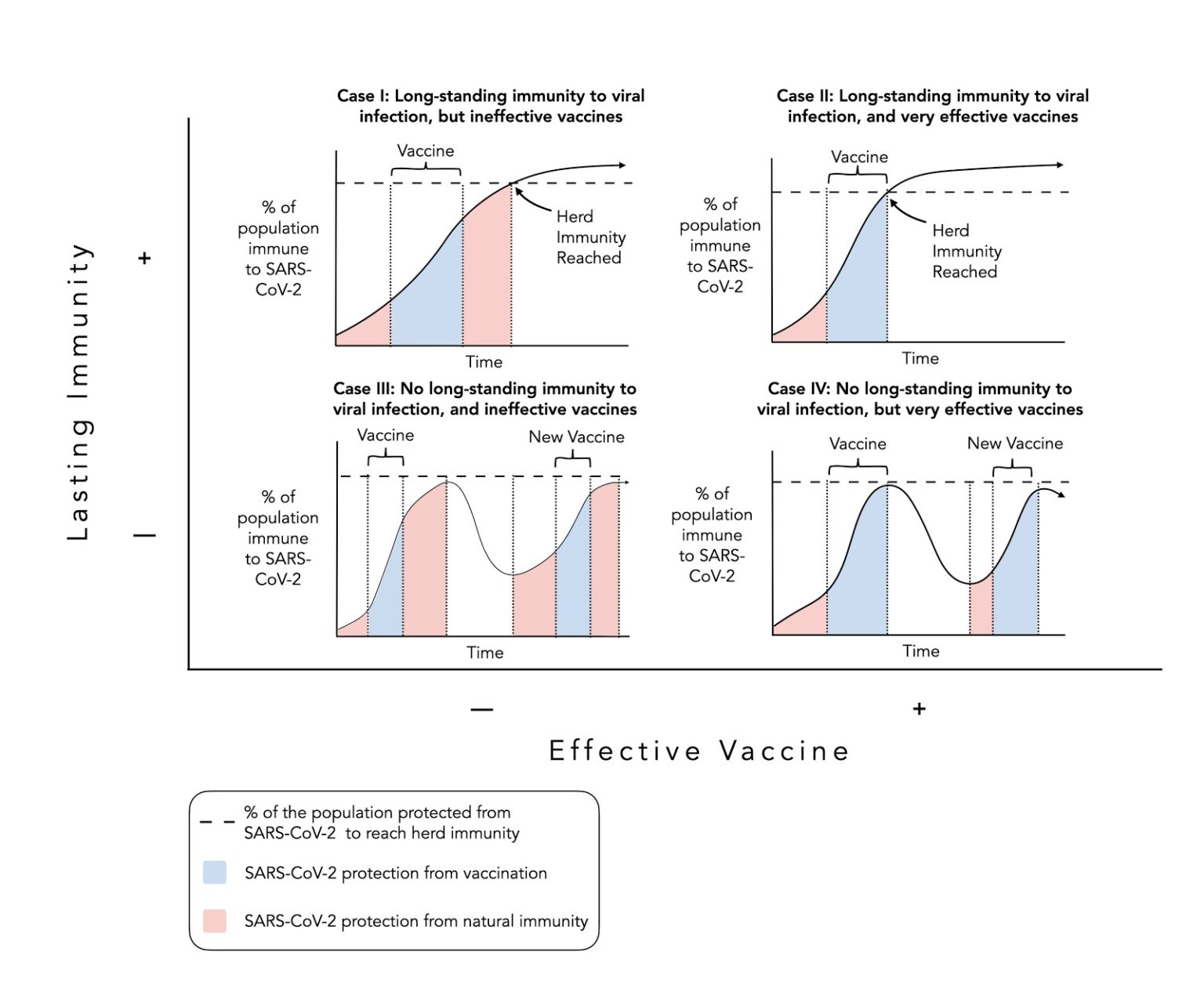
Peter Attia, another medical doctor and clinician, published a chart that I found interesting when trying to predict the various ways the pandemic could play-out. It's a two-by-two matrix with how long protective immunity lasts after disease or vaccination, and how effective the vaccine is. The best case is a vaccine that works great and lasts a lifetime (Case II). But we see cases III and IV, where we never get herd immunity.
Nobody knows which of these (or even some other variant) will happen, but it's interesting to think through these possibilities. To read Attia's comments on the slide, that's here: https://peterattiamd.com/covid-framework-how-does-this-thing-end/
